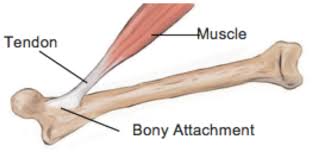
PRP (or platelet rich plasma) has become an intervention offered by the medical profession to stimulate the healing of persistent pain related to tendon and joint injuries over the last few years.
What is PRP?
PRP involves taking your own blood from a vein (normally in your arm) – which is then placed in a centrifuge and ‘spun down’ to separate the blood into 3 products – red blood cells, platelet poor plasma, and platelet rich plasma.
The last item – the PRP – is kept, and injected into the affected tissue, with the thought being the ‘growth factors’ have a benefit in prooting tissue healing.
What does the evidence show?
Unfortunately the majority of the research on PRP has been done with poor research design - so there is a lot of confusing data out there and we need to use caution when interpreting the results.
Tennis Elbow
This systematic review showed strong evidence against platelet-rich plasma injections for chronic lateral epicondylar tendinopathy.
Another study concluded that data in this review do not support the use of autologous blood or PRP injection for treatment of lateral elbow pain.
Hip osteoarthritis
This study showed no difference between saline injections and PRP.
Achilles Tendinopathy
This study showed no proof that PRP injections can enhance patient functional & clinical outcomes for Achilles tendinopathy.
Plantar Fasciitis
This study showed strong evidence indicates that autologous growth factor injections do not improve plantar fasciopathy pain or function.
My advice:
If you have been suffering with persistent tendon or joint pain and are considering PRP, I would encourage you to do a 8-12 week trial of active physiotherapy to promote healing.
This would take a holistic view of healing with a primary focus on increasing the bodies natural capacity for healing:
getting extra aerobic exercise particularly focused on Zone 2 where you are getting your heart rate up but not above your threshold (aiming for 150 minutes per week)
promote extra sleep - aiming for 7-9 hours of quality sleep
eating a highly nutritious diet with increased dose of protein and collagen rich foods to help tendon repair
avoid all compression loads to the tendons - including stretching and deep tissue massage directly over the tendon
relative rest of the tendon - reducing large spikes in load but still maintaining some activity to allow for the healing
if PAIN is your most pressing issue, take the time to LEARN about the complexity of the pain experience. When you understand that fear, anxiety and uncertainty can directly contribute to your pain then you can see other options for treatment beyond trying to ‘fix the body’. Assuming the body is a simple machine that breaks down and then causes pain is a very limited view and traps you in state of fragility. You can experience pain without ANY specific tissue damage - this can be an absolute game changer and get your healing on the fast track.
Yes this approach is boring and doesn’t promise the idea of a ‘quick fix’ –it takes time, patience and belief in the human body to heal given the right environment.
If you doctor is promoting PRP as an ‘evidence-based procedure’ then alarm bells should be going off. As that is not a factual statement.
Instead, your doctor should LISTEN to you and focus on YOUR SPECIFIC NEEDS to help you get better - that is called patient-centered care and involves getting to know your goals, fears, understanding of the problem and capacity to heal with your current lifestyle.
The bottom line
PRP may turn out to be a useful adjunct to treatment of persistent tendon and joint pain.
More research is required to confirm which patients are most suitable as currently results are unreliable.
As most PRP protocols suggest a period of relative rest from 2-8 weeks afterwards, it is difficult to know how much improvement is from the PRP vs rest and time.
I would advise PRP should be used only after a holistic and person centered physiotherapy program is performed for 8-12 weeks.
The best treatment effects may occur when the patient is a the center of the process of informed consent, shared decision making and actively doing things that support healing through a healthy lifestyle.
My prediction is that PRP used in isolation to try and ‘fix the pain’ and stimulate healing will be a very limited benefit.