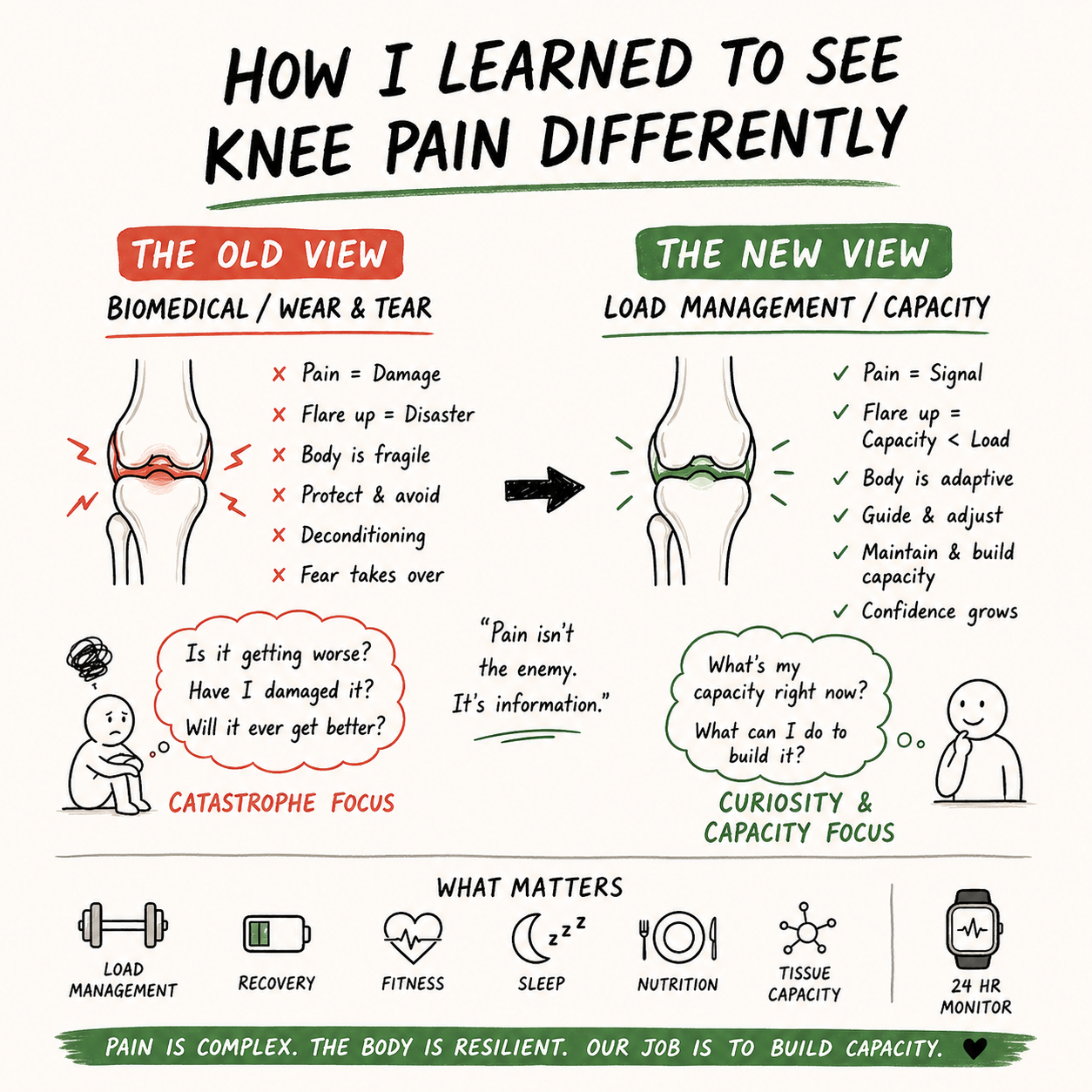
Why “Making Sense” Has Been So Confusing
If you’ve had persistent pain, chances are you’ve been on a journey to make sense of it.
At first, the story is simple:
“Something is damaged.”
That’s the traditional biomedical model.
Find the structure.
Fix the structure.
Problem solved.
And to be fair — that model worked incredibly well for many things:
fractures
infections
surgical emergencies
major tissue injuries
But when it came to persistent musculoskeletal pain, the picture became far less clear.
A huge percentage of people continued to have pain long after tissues were expected to heal.
Around 1 in 5 adults now live with chronic pain.
Many people with back pain, neck pain, tendon pain or knee pain never fully returned to normal despite scans, treatments, injections or even surgery.
In some cases, the endless search for “the damaged part” may have even amplified fear, hypervigilance and disability.
That’s when cracks started to appear in the old paradigm.
Then Came the Big Shift
Over the last 10–15 years, a new model took over.
Pain wasn’t about damage anymore.
It was about the brain.
This shift—driven by researchers like Lorimer Moseley—was huge.
And to be fair, it helped a lot of people.
For many, it was a necessary correction.
But Something Strange Happened
The PNE model quickly became the dominant narrative in modern pain rehabilitation.
Because it was linked to neuroscience and the brain, it carried an immediate sense of authority and sophistication.
In some circles, it almost became assumed that a “brain-based” explanation must automatically be more advanced and more correct.
But as time went on, many clinicians and patients quietly started noticing something important:
understanding pain intellectually didn’t always translate into meaningful recovery physically.
And like most dominant ideas, it started to stretch beyond its limits.
Pain became explained as:
“Your brain is overprotective”
“Your nervous system is misfiring”
“It’s a learned response”
For some people, this clicked.
For others, it didn’t.
The Quiet Frustration
If you’re in that second group, you might recognise this:
You understand the explanation
You agree with it intellectually
But your body hasn’t changed much
And when it doesn’t work, the explanation subtly turns back on you:
That’s a tough place to be.
Because now you’re not just in pain…
You’re also not doing the model properly
A Line That Stopped Me in My Tracks
Reading Nassim Nicholas Taleb, I came across this:
“When it comes to narratives, the brain seems to be the last province of the theoretician-charlatan… Add ‘neuro’ to something and it suddenly becomes more convincing… yet the brain is too complex for that.”
That hit hard.
Because it explained something I had been feeling for years but couldn’t articulate.
The Problem Wasn’t That PNE Was Wrong
It’s that it became too neat.
Too explanatory.
Too confident.
As if we could reduce something as complex as pain to:
“The brain thinks you’re in danger”
That’s a compelling story.
But it’s still… a story.
The Shift That Changed My Thinking
Then I came across the work of neuroscientist Bud Craig.
And his book How Do You Feel?.
It didn’t give me a better story.
It gave me something more useful:
A way to stop over-explaining… and start observing
A Different Kind of Understanding
Craig’s model is simpler, but deeper:
Pain is a feeling that reflects the state of your body.
Not just your brain.
Not just your tissues.
Your whole system.
This Changes Everything
Instead of asking:
“Why does my brain think I’m in danger?”
You start asking:
“What is my body actually dealing with right now?”
load
fatigue
stress
poor sleep
deconditioning
inconsistent movement
Pain becomes less about interpretation…
…and more about capacity vs demand
Less Theory, More Reality
This is where Taleb’s thinking becomes useful again.
He writes about avoiding over-explanation and focusing on:
Noticing the PATTERNS in your body over time
In other words:
What happens when you walk more?
What happens when you sleep better?
What happens when you overload your system?
Not in theory.
But in reality.
This Is the Shift
From:
“What does this pain mean?”
To:
“What does my system do in response to what I’m doing?”
How I Work Now (Because of This)
I’m far less interested in:
And far more interested in:
We Use Simple Anchors
Not guesswork.
Things like:
Because your body doesn’t lie.
No Ideology. Just Feedback.
We’re not trying to:
fix a structure
retrain a brain
We’re trying to:
help your system handle more… and see what happens
Why This Feels Different
Because it removes pressure.
You don’t need to:
You just need to:
observe, adjust, and build capacity
Final Thought
The biggest shift in pain isn’t from body → brain.
It’s from:
theory → reality
Takeaway
Pain is not something you need to perfectly understand.
It’s something you need to work with.
And the more your system can handle…
The less it needs to shout.